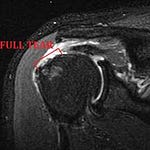
Earlier this week media reported that Robert F. Kennedy Jr., the Secretary of Health and Human Services, had surgery to repair a torn rotator cuff.
That’s interesting. Not just because I wrote about rotator cuff surgery last week.
Kennedy has spent years arguing that medical treatments should be recommended only after they’re proven to work in rigorous trials.
Which raises the inevitable question: What do rigorous trials show about rotator cuff surgery?
At half a million performed each year in the U.S., rotator cuff surgery is among the most common orthopedic procedures. Which is curious, because the handful of randomized trials testing it have repeatedly found little or no difference between surgery and physical therapy. Even within orthopedics there is deep skepticism, and sham-controlled trials of the procedure are currently underway.1
Meanwhile, as I discussed last week, in a recent MRI study of healthy Finnish people age 40 and over, fixable ‘injuries’ were seen in perfectly functional shoulders. And not just some of them: 96% of people with no shoulder complaints had potentially surgical lesions. Tendon tears, present in 80% of study participants in Kennedy’s age group, appear to be little more than a normal sign of aging. Like wrinkles in the rotator cuff.
In contrast, for years Kennedy has argued vaccines should not be recommended unless they’re supported by randomized trials. He has suggested the evidence base is shaky, with poor documentation of harms, and that vaccines are overused, driven by corporatized medicine and windfall profits.
To me, these are legitimate concerns. I see it as quite sensible to scrutinize the trials that underlie current practice. I believe skepticism about such evidence is admirable, and I believe his call for transparency is righteous. Medicine has adopted many treatments too quickly, often on the slimmest of data, with no avenue for patients to know or weigh in.
But RFK Jr.’s critiques of seminal vaccine data are, comparatively, small time. They boil down to methodologic details in trials that found benefits. Issues such as placebo selection, evolving formulations, and long-term follow-up are reasonable concerns worth airing and discussing—but they’re nit-picky.
In stark contrast, red flags in the data on rotator cuff surgery are big time: namely, the surgery didn’t work—there was no benefit. That ain’t a nit-pick.
To be fair, one man’s shoulder treatment does not carry the same implications as childhood vaccine policy. But this man made a name debating the fine print in vaccine trials. RFK Jr. having shoulder surgery is like Mohatma Gandhi having road rage.
Moreover, just last year the Secretary openly recognized that American healthcare wrongly incentivizes costly, often dubious elective surgeries—a crucial insight that helps explain why orthopedics is disproportionately lucrative and why unproven surgeries like rotator cuff repair are the cash cow of the specialty.
Based on this insight, Kennedy suggested shifting incentives away from such elective surgeries and “toward primary care and prevention.”
Yet now, when Kennedy became a patient, the calculus appears different. Faced with shoulder pain and an expert’s recommendation, he did not turn his own famously cutting eye on the data. Which may be a serious mistake. For a 72-year old man the risks associated with surgery (heart attack, stroke, pneumonia, blood clots, death) are greater than any benefit found in a trial of rotator cuff surgery. And in light of the Finnish data, the notion that whatever MRI finding his surgeon is targeting is the true cause of his shoulder problems is, at best, highly suspect.
All of which means that RFK Jr.’s decision to undergo surgery rests not on evidence, but on the advice of experts.
That’s interesting, too.
This same Secretary of Health recently said “Trusting the experts is not a feature of democracy and it’s not a feature of science. It’s a feature of religion and totalitarianism.”
I agree.
But evidence, it seems, is most powerful when it governs other people’s care.
Sham controlled surgery trials tend to be performed when no objective proof of a procedure’s effectiveness can be found, and critics suspect that the pain and function improvements often seen after the surgery are either a placebo effect or else no better than natural healing would produce. Historically, sham-controlled surgery trials virtually always find no benefit. It’s a good bet that rotator cuff surgeries will be no different, but one can never know until the trials are done.